Is Running Bad for Your Discs? What Current Research Actually Says
For years, runners with back pain have been told some version of the same thing:
“Running is bad for your back.”
“It’s wearing out your discs.”
“You should probably stop running.”
For someone who has spent their life being active, that advice can feel frustrating, especially if running is part of how you stay fit, manage stress, maintain energy, and keep yourself performing at a high level.
The good news is that the current research does not support the idea that running automatically damages the discs in your spine.
In fact, some studies suggest that regular, appropriately progressed running may be neutral to mildly beneficial for disc health. That does not mean running is a cure for disc problems, and it does not mean every person with back pain should immediately increase their mileage. But it does challenge the outdated belief that running simply “wears out” your spine.
What Are Spinal Discs?
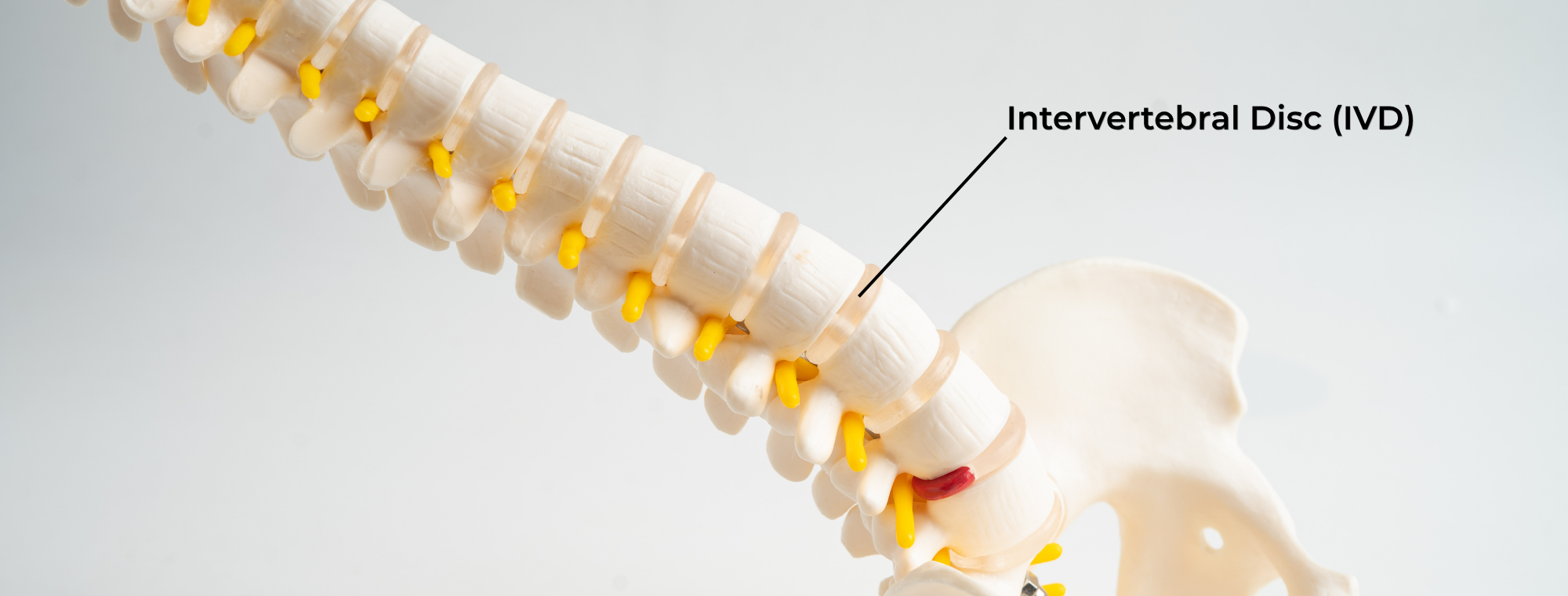
Intervertebral discs are the structures located between the bones of the spine. They help absorb load, allow movement, and distribute force through the spine.
You can think of them as living tissues that respond to stress, movement, and loading, not just passive cushions that slowly break down every time you move.
Researchers often study disc health using MRI-based measurements such as disc height, hydration, proteoglycan content, and signal intensity. These markers are not perfect, but they help researchers understand how discs may adapt over time.
The Old Belief: Running Wears Out Your Discs
It is easy to see why this belief became so common.
Running involves repetitive impact. Every step creates load through the legs, hips, pelvis, and spine. So it makes sense that many people assume more impact must equal more disc damage.
But the body is more complex than that.
Muscles, bones, tendons, cartilage, and discs all respond to the right amount of load. The key question is not whether running loads the spine. It does.
The better question is:
Is that load harmful, helpful, or simply too much for what your body can currently tolerate?
That distinction matters, especially for active adults who do not want to be told to stop moving every time they experience pain.
What the Research Shows
A 2017 study published in Scientific Reports compared long-distance runners, joggers, and non-athletic adults. The researchers found that chronic running was associated with better disc composition, including markers related to hydration and proteoglycan content.
They also found that fast walking and slow running appeared to correlate with more favorable disc characteristics, while lower-intensity activity, static positions, and high-impact tasks did not show the same relationship.
This study is important because it suggests that the spine may respond positively to certain types of loading. However, it is also important to be accurate: the study showed an association. It did not prove that running directly caused healthier discs.
A 2024 systematic review in Sports Health looked at 13 studies with 632 participants. The review found that running can cause short-term changes in disc measurements after a run, likely due to temporary compression and fluid movement out of the disc. However, cross-sectional studies suggested that long-term running may have a mild positive effect on disc health.
A 2026 systematic review and meta-analysis in Sports Medicine found that upright loading, mostly running, was associated with better intervertebral disc health compared to controls. Running was the only physical loading exposure associated with better disc health in that analysis. However, the authors rated the certainty of evidence as very low and emphasized that more prospective running studies are needed before stronger conclusions can be made.
A 2026 secondary analysis of the ASTEROID randomized trial looked at disc adaptations during a 12-week progressive run-walk program in adults with chronic low back pain. This does not mean running directly repairs discs, but it does support the idea that progressive running can be studied as a potentially tolerable form of loading in people with chronic low back pain.
What We Can Reasonably Say
Based on the current research, it is reasonable to say:
Running does not appear to be automatically harmful to healthy spinal discs.
Regular running may be associated with better markers of disc health, especially compared to a less active lifestyle.
Short-term disc compression after running is expected and does not necessarily mean damage has occurred.
The evidence is still developing, so we should avoid claiming that running definitively “strengthens” or “repairs” everyone’s discs.
The ideal amount, speed, frequency, and intensity of running for disc health is still unclear.
A more accurate summary would be:
Current evidence suggests that regular running is not inherently damaging to spinal discs and may be associated with better disc health markers, but more high-quality long-term research is needed to understand cause, effect, and ideal training dosage.
What We Should Not Overstate
It would be too strong to say:
“Running fixes disc degeneration.”
“Running prevents disc herniations.”
“Everyone with a disc bulge should run.”
“More running always means healthier discs.”
The research does not support those claims.
This is where the conversation needs more nuance. For one person, running may be a helpful and tolerable form of exercise. For another person, their current running volume, intensity, terrain, or recovery habits may be exceeding what their body can handle right now.
That does not always mean running is the problem.
It may mean the dose is the problem.
Why Dose Matters
Loading is not simply good or bad. The amount, frequency, intensity, and timing all matter.
A gradual run-walk program is very different from suddenly increasing mileage, adding speed work, running downhill, or pushing through symptoms that are clearly getting worse.
For many runners, back pain does not mean running has to stop forever. It may mean your current training load is greater than your body’s current capacity.
That can happen for several reasons:
Too much mileage too soon.
Not enough recovery between runs.
Weakness or mobility limitations in the hips, trunk, or lower body.
Long hours of sitting combined with high training demands.
A recent flare-up that needs temporary modification.
More stress from hills, speed work, harder surfaces, or poor sleep.
In other words, the goal is not always complete rest.
Often, the goal is finding the right entry point and building from there.
What This Means If You’re a Runner With Back Pain
If you have back pain and enjoy running, this research should be encouraging.
Running is not automatically bad for your spine.
That being said, symptoms still matter. If running increases your pain, causes symptoms into the leg, worsens numbness or tingling, or makes normal daily activities harder, it is worth getting assessed.
For some people, the first step may be walking. For others, it may be short run-walk intervals. For experienced runners, the answer may be modifying mileage, intensity, terrain, strength training, or recovery rather than stopping completely.
This is where a structured return-to-running plan can be helpful. Instead of guessing when to rest, when to run, or how much to progress, the goal is to identify what your body can currently tolerate and build from there.
Our Approach at Resolve Chiropractic
At Resolve Chiropractic, we work with active adults who want to keep moving, training, and performing, not simply avoid everything that causes discomfort.
Our goal is not to create fear around running or exercise. At the same time, we do not want you pushing through symptoms without a plan.
For runners with low back pain, we look at the full picture:
How your spine, hips, and pelvis are moving.
What your current training load looks like.
Whether your symptoms are improving, worsening, or staying the same.
How strength, mobility, and recovery may be affecting your tolerance.
What modifications would allow you to keep moving safely.
For patients who need more structure, our 6-week Return to Running Program is designed to help you rebuild running tolerance in a progressive, personalized way. This may include run-walk programming, strength work, mobility work, soft tissue treatment, spinal care, training modifications, and guidance on how to safely increase volume or intensity.
The goal is simple:
Help you reduce pain, improve capacity, and get back to running with more confidence.
Bottom Line
Running is not automatically bad for your discs.
The current research suggests that regular, appropriately progressed running may be associated with healthier disc characteristics. However, the evidence is still developing, and we should be careful not to overstate the findings.
The most practical takeaway is this:
Your spine is designed to respond to movement and load. The key is finding the right amount of running for your current body, symptoms, and goals.
If back pain has been keeping you from running, or if you are unsure how to safely return after an injury, we can help you build a plan that gets you moving in the right direction.
References
Belavý DL, Quittner MJ, Ridgers ND, Ling Y, Connell D, Rantalainen T. Running exercise strengthens the intervertebral disc. Scientific Reports. 2017.
Shu D, et al. Impact of Running Exercise on Intervertebral Disc: A Systematic Review. Sports Health. 2024.
Samanna CL, et al. The Impact of Exercise on Intervertebral Disc Health: A Systematic Review and Meta-Analysis. Sports Medicine. 2026.
Samanna CL, et al. Running is associated with intervertebral disc adaptations: a pre-planned secondary analysis of the ASTEROID randomised controlled trial. European Spine Journal. 2026.